[This is Chapter 2 of From Killer to Common Cold, which was deplatformed from Amazon in 2020. Posting for posterity.]
Chapter 2: What Does a Virus Want?
Viruses are explosive.
They are an aggregation of proteins and genetic material with a single goal—to make more of themselves. Viruses literally blow the cell they are trapped inside up in order to escape. When given enough resources, they demonstrate exponential, explosive growth. Remember that viruses, unlike bacteria, protozoa, and fungi, aren’t even alive. They are the ultimate parasites that require a living organism—often you—to survive and reproduce.
SARS-CoV-2 is the virus that causes COVID-19. The “CoV” stands for coronavirus, which is a large family of closely related viruses that cause various illnesses in many different species. We will learn about the human coronaviruses in Chapter 4, but first, we’ll discuss what exactly a virus is and how it interacts with its host.
Viruses are small—much smaller than even bacteria. They are the ultimate minimalists, carrying only what they need to get from one host to another. They must do three basic things. First, they must transfer from host to host via the environment. Then, once in a host, they need to spread from cell to cell. In the cell, they make copies of themselves.
Viruses take over the metabolic machinery of a cell and then make so many copies of themselves that they obliterate the cell. Next, they find another cell to infect. Within a host, only the host’s immune system can break this chain of cell-to-cell transfer.
Surviving in the environment outside the host, however, is difficult. The virus must leave a host (usually via sneezing, coughing, or diarrhea) and get onto, and then into, another host. The environment is a hostile place for viruses. They are diluted by space and time and desiccated by sunlight. If they land on the wrong type of host, it is all for naught. A virus infects one species of animal.
To protect themselves from the environment, enveloped viruses use a lipid membrane to coat themselves. Not infrequently, viruses actually use your own cell’s lipid membrane to do so. Clever! They use your cellular machinery to replicate, and your cell’s membrane as a coat. They are minimalists, but not ideal houseguests.
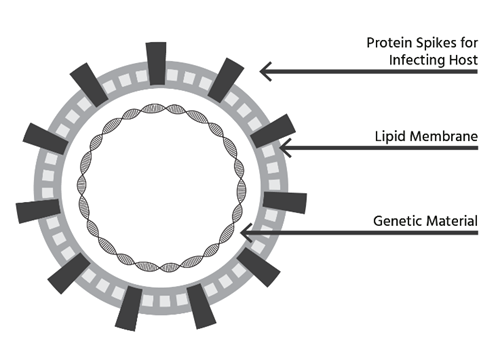
Image adapted from “Why Soap Works” by Jonathan Corum and Ferris Jabr, New York Times, 3/13/20.
Next, small protein spikes protrude from the virus and latch onto your cells. The proteins that extend from coronaviruses resemble the solar corona in electron micrographs, which is why they are named that way. These protein spikes attach like a lock and key to receptors on your cells. Although these receptors serve other functions, the virus learns to exploit them to gain entry. A virus uses its protein spikes to bind to your cell’s receptors, enabling it to enter the cell. Once inside, the virus hijacks your cellular machinery to produce more copies of itself.
Viruses have either RNA or DNA as their genetic material. RNA viruses mutate more rapidly and possess some extra proteins to replicate. We can sometimes target those extra proteins with medications, which make RNA viruses slightly more treatable.
Coronaviruses are large, enveloped RNA viruses. They are found in many different animal species and cause different syndromes in different animals. Cows and pigs get diarrhea from their versions of coronavirus, whereas other species can have respiratory, neurological, and asymptomatic illnesses.
Humans are constantly exposed to animal coronaviruses. However, because the virus is adapted to living in its host species, most of the time it cannot attach to human cells. A mutation in the protein is needed to allow it to bind effectively to the new host’s receptors, similar to a lock and key.
SARS-CoV-2 likely started in bats, but we are still not entirely sure. The ancestor of SARS-CoV-2 could cause a cold, diarrhea, or no symptoms at all in bats. Then, randomly, a mutation happened in the spike proteins in the ancestor virus that allowed the virus to spread from bats to humans. This step may actually have happened through an intermediary—a third animal species. The mutation allowed the spike protein of SARS-CoV-2 (which used to only latch onto bat cells) to latch onto human respiratory cells. From this random mutation in a bat coronavirus, the pandemic began. [2025 update: It was a lab leak]
A genetic change in the spike protein of SARS-CoV-2 enabled it to bind to human respiratory cells and enter them. Once inside, it hijacks our cells’ reproductive machinery to make more copies of itself. These copies are then released locally and infect other nearby cells. The process leads to exponential growth until the virus exhausts its resources or the immune system halts it. Remember, SARS-CoV-2 aims to spread to new hosts so it can infect others and keep replicating. To promote spreading to new hosts, the virus causes symptoms. Symptoms like coughing or sneezing spray the virus into the environment, where it may attach to a new person’s respiratory cells, continuing the cycle of person-to-person transmission.
Viruses that mutate and jump species from animals to humans are called zoonotic viruses or zoonoses. Usually, humans are dead-end hosts because the virus can’t spread from person to person. It is hard for a virus to learn how to bind a new receptor, replicate in a new species, and spread effectively. That’s why pandemics are relatively rare, even though humans are constantly exposed to animal viruses. However, when a virus does jump to humans and can spread easily from person to person, watch out world.
The immune response to this is complex, to say the least. The immune system is, perhaps after consciousness, the most complicated concept in medicine. Each individual has a slightly different immune system, but each of us has specific and non-specific responses.
The non-specific response is pretty easy to picture, as you have experienced it many times. When your body is worried that something is going on, perhaps an invader is on board, it dumps out cytokines and other immune-modulating molecules as the initial phase of host defense. You feel faint, fatigued, hot, sweaty, and tired. This is all your body’s way of saying, “Hey, get ready!” Fever is part of the non-specific host defense response. Your cells tolerate higher body temperatures more readily than the invaders. This non-specific response primes your cells for a fight and may ward off an initial infection. Usually, a non-specific response gives your cells a fighting chance to defend themselves and prepares your body for the specific immune response.
After a few days, your body processes the virus and makes specific antibodies against viral proteins. B-cells produce antibodies and are one arm of specific immunity. Antibodies can be detected in blood tests. The antibodies coat the spike proteins of the viruses and prevent them from attaching to new cells. If you have them, it usually implies you are immune to the specific infection.
In reality, it is a little more complicated than that. For example, HIV easily survives outside of cells even when there are plenty of antibodies. In addition, anti-coronavirus antibodies wane over time and may or may not protect you from future infection. When considering coronavirus infections, immunity due to specific antibodies is usually neither permanent nor long-lived.
In addition to antibodies, the cellular immune system is another part of the specific immune response. The cellular immune system destroys cells infected by a virus. To simplify, different T-cells coordinate your cellular immune response. Some T-cells detect infected cells and kill them, stopping the production of more virus. Other T-cells serve as the conductor of your immune orchestra. Finally, memory T-cells remember past infections and respond quickly when you encounter a similar virus antigen again.
The immune system is made up of many parts and varies from person to person. We all have slightly different immune systems that may be more or less effective at fighting various infections. Now, consider this question, which will be answered later: Could some people in the population naturally be better at fighting off Covid-19 just by chance? [2025 thought: This was not allowed to be discussed when this book was written. We now know that fat, unhealthy people are the reason why the USA had such high relative mortality rates from covid.]
The relationships between viruses and their hosts are complex. In nature, invaders and hosts gradually develop an understanding. For their native species, a viral infection is often mild or even shows no symptoms. Usually, only when a virus jumps species does it tend to cause widespread death and destruction. That is what an epidemic is: a new infection leading to significant loss of life. Remember, the goal of a virus is to produce more copies of itself. A dead host is a dead-end host—no more virus can be produced. More efficient transmission usually involves causing only mild illness, which gives the virus more chances to spread to other hosts. A virus aims to be benign because, in most cases, that is the best way to replicate and spread.
That a virus wants to reproduce itself is a tautology — it is true because it is true. If the virus didn’t reproduce itself, it wouldn’t be here to do so. It wouldn’t exist. We, in turn, wouldn’t know it was there and wouldn’t ask why it exists.
Ultimately, replication is what all lifeforms “want.” Understand that this is not a conscious desire, but rather a just-so story. This tautology is a fundamental principle of evolutionary biology. A replicating element replicates—that’s why it exists to observe. This applies to all replicating organisms or lifeforms.
Evolutionary biology studies how things change over time in replicating entities like humans and viruses. In infectious diseases, we observe evolution in real time, such as bacteria developing resistance to antibiotics or HIV becoming resistant to prescribed therapy. In humans, the effects of evolution are much slower. Often, human behavior influences evolution more than genetic changes do. However, evolutionary biology is a complex topic for a different book.
In the survival of the fittest, the most successful COVID-19 virus is the one that makes the most copies of itself. Certainly, we will observe genetic changes in SARS-CoV-2 that affect its ability to replicate. Evolutionary biology can help both humans and SARS-CoV-2 achieve our goals. Through behavioral changes, humans can suffer and die less from infection, and SARS-CoV-2 can evolve to reproduce more. Believe it or not, as a new host to SARS-CoV-2, humans need to assist, rather than hinder, SARS-CoV-2 in reaching its goal. A benign virus is a good virus.