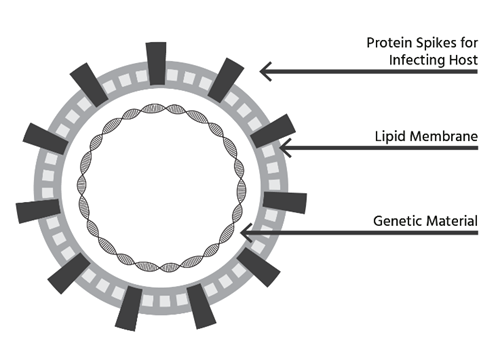
Eradication is Impossible
Herd immunity is not the goal; herd protection is. After all, eradicating Covid-19 is impossible, so there’s no reason to aim for herd immunity. Instead, we need to stop the epidemic transmission of Covid-19, which endangers our healthcare and public health resources. Once we overcome regional epidemics, we move on to the Transitional Phase.
Covid-19 is a pandemic with multiple simultaneous epidemics worldwide. In the U.S., discussions usually focus on the national or state level, with ‘hot spots’ adding to case counts. However, viewing the U.S. as a whole is unhelpful because there are many regional epidemics, not a single one. Despite shared borders and resources, regional differences are significant. For example, California’s urban areas and rural farmland differ greatly from New York City or New York State, making direct comparisons misleading.
I find it most useful to view the pandemic as multiple co-occurring epidemics in specific regions. Since healthcare and public health resources are organized regionally, epidemics should also be considered on a regional basis. Currently, American healthcare systems mostly operate independently, though regions can receive support from their state or the federal government. This facilitates accurate case reporting and targeted responses within relatively uniform areas. However, each region differs in geography, population density, resources, and vulnerable populations, meaning they will benefit differently from mitigation measures aimed at controlling new infections.
Before we can even consider eradicating Covid-19, we must eliminate it from individual regions—region by region. Elimination refers to eradicating a regional epidemic. Before we wipe out a pandemic, we need to eliminate one epidemic after another.
It is said: think globally, act locally. In a pandemic, there are no more accurate words. While it is true that the rest of the world is just a plane ride away, we must start by thinking locally to manage the pandemic.
Regional Epidemics
Let’s dive in and explore how we can effectively combat our regional epidemic. How can we achieve herd immunity regionally and stop the spread of the disease in your area? Remember, herd immunity is helpful when managing an epidemic that can be controlled within regional populations through vaccination. It’s important to understand that when herd immunity is complete, it can lead to the regional elimination of a virus. If elimination occurs worldwide, the virus can be eradicated entirely. This is what happened with smallpox and rinderpest, the only two diseases we have successfully eradicated. These viral diseases are now extinct in all populations but remain stored in research and bioterrorism labs. We no longer need to vaccinate against smallpox in humans because it has been eradicated globally. Rinderpest, a disease affecting cattle and other ungulates, was eradicated through vaccination and surveillance.
More commonly, however, vaccination and herd immunity lead to the elimination of a virus. Instead of making a virus completely extinct or eradicated, elimination means that the virus no longer circulates in a specific regional population. The virus, however, remains present in other human populations. Polio, measles, and mumps are examples of viral diseases that have been eliminated from highly vaccinated pockets of people but still exist in populations where we cannot vaccinate enough individuals to achieve local herd immunity.
Covid-19 is a completely different story. Because immunity from Covid-19 is neither long-lasting nor complete, vaccination won’t lead to local elimination or eradication. Even with effective vaccines against SARS-CoV-2, we know immunity will decrease over time, and Covid-19 will keep circulating regionally. In other words, eradicating Covid-19 is impossible. Whether we have a vaccine or not, or effective treatment or not, Covid-19 will cause human disease indefinitely.
To illustrate why eradication is impossible, let’s examine the specific criteria for considering a disease eradicated. Eradication is defined as the permanent reduction to zero of worldwide infection rates caused by a specific agent through deliberate efforts. A virus that can be eradicated from humans must (1) have no non-human reservoirs, (2) be easily recognizable and have an effective treatment or vaccine, and (3) have a global desire and effort to eliminate the disease.
The first reason is why MERS, which is also a coronavirus, will never be eradicated. MERS resides in camels, and we are not willing to euthanize all camels worldwide just to eliminate MERS. However, humans are not the preferred hosts for MERS. Although we are occasionally affected by this highly deadly disease, we are mostly dead-end hosts for MERS. It does not easily spread from human to human.
SARS-CoV-1 (which causes SARS) and SARS-CoV-2 (which causes Covid-19), on the other hand, both jumped species from bats. Neither are found in bats anymore, so we don’t worry much about bats triggering another round of CoV-1 or CoV-2. However, note the nomenclature: 1, 2… What comes next? Many bats and other species carry non-human coronaviruses and may jump species, causing new pandemics. But that is a different story.
With SARS-CoV-2, there may actually be no non-human reservoirs of this virus. Of course, cats, dogs, lions, tigers, alpacas, and mink have all been diagnosed with Covid-19. But hopefully, these are dead-end hosts (like humans are for MERS) rather than potential reservoirs.
Covid-19 could probably be eradicated based on the first criterion of having no non-human reservoir species. However, eradication requires both an effective treatment or preventive measure and easy recognition. Additionally, eradicating a disease demands global desire and effort. Covid-19 fails to meet these last two criteria, as discussed below. SARS-CoV-1 and smallpox provide insight into why we cannot eradicate SARS-CoV-2.
SARS-CoV-1, the virus that causes SARS, has been removed from human populations. However, it has not been officially declared eradicated because of concerns about intentional or accidental release from laboratories. Aside from the freezers in biocontainment labs, SARS-CoV-1 probably has no current natural reservoir. SARS has no treatment or vaccine, but it is relatively easy to control because it only spreads once symptoms appear. Additionally, if you are worried about seeing SARS cases—such as if there was a known lab release—it is relatively straightforward to diagnose. There is no asymptomatic or pre-symptomatic transmission. Therefore, with no reservoir for SARS, it is easy to diagnose and contain. Global cooperation also contributed to its elimination from all human populations.
Smallpox, once again, has been eradicated. It has no non-human reservoir and is easy to diagnose, as the pox is visible from across the room. Additionally, there is an effective preventive measure (vaccination), and after having the disease, you are immune (and usually scarred) for life. Smallpox checks all the boxes, which is why it was eradicated.
Covid-19 fails the last two criteria for eradication. Not only is diagnosis difficult because of asymptomatic and pre-symptomatic transmission, but also Covid-19 is clinically indistinguishable from many other respiratory infections. If someone presents with fever, chills, and a cough, it could be one of hundreds of infectious or non-infectious conditions that resemble each other without diagnostic testing. Even once we develop rapid, reliable, point-of-care tests for Covid-19, asymptomatic and pre-symptomatic transmission remains a concern. Currently, there is neither effective treatment nor adequate preventive measures.
It may be possible that we never find a truly effective treatment for Covid-19. Historically, we have not yet developed an effective treatment for a respiratory virus, let alone a treatment for an asymptomatic respiratory virus. There are drugs with modest effects against influenza, and these drugs also work to prevent influenza before exposure. But how do you treat someone who is just colonized by SARS-CoV-2 (asymptomatically infected) but not ill from Covid-19? Is it possible to treat someone who is not sick? As discussed in Chapter 2, drugs are hard to develop for viruses because they use your own cells to replicate. Medications tend to have side effects, which make them undesirable to use when you feel fine but have SARS-CoV-2 replicating in your nose and lungs. We will certainly develop additional drugs against Covid-19, but no one sees pharmaceuticals as a silver bullet.
Regarding vaccination, the chances are high that most people who choose to get vaccinated will develop some level of immunity. However, it is unlikely that we will create a vaccine that offers complete and long-lasting protection. None of the other human coronaviruses cause permanent immunity, even after natural infection. Immunity tends to be temporary, and similar to the common cold coronaviruses, re-infection is expected after some time. This is true following natural infection and probably will be the case after vaccination as well.
Regarding preventative measures, if everyone could live in a bubble for six weeks, we might be able to stop nearly all transmission of Covid-19. Can you envision a method to accomplish this globally within a six-week timeframe? This isn’t a realistic option for such a highly contagious virus. In fact, SARS-CoV-2 can persist in immunocompromised individuals for weeks. Any leftover virus would likely reignite the outbreak once the bubble burst.
Let’s do a thought experiment for a second. Assume we have a vaccine for Covid-19 that is 100% effective and lasts for at least two years. This is unlikely, as no vaccine is 100% effective. If we vaccinate every man, woman, and child in the world within two years, we can eradicate Covid-19.
What about those people who refuse vaccination or live in hard-to-reach areas of the world? This is why we haven’t eradicated hepatitis A, hepatitis B, polio, measles, mumps, and rubella. All of these infections have a single host—humans. They can be eliminated, but they haven’t been yet. Even if there is an effective treatment or vaccine, imagine distributing it worldwide at the same time, let alone getting everyone in the United States vaccinated 100% of the time.
Since we cannot eradicate Covid-19 based on eradication criteria, it is clear to me that Covid-19 will continue to circulate in human populations. It will become endemic—present continuously in low amounts. Covid-19 as a pandemic will end, but it will not be eradicated. It will go from epidemic to endemic.
There is an example in our shared history where this has already occurred. Now, let’s examine the period in human history when a human coronavirus caused an epidemic and has since become endemic.