For people under 20, the attack rate is approximately 20% after exposure. For individuals over 70, the rate of infection is approximately 70% after exposure.
Chapter 6: NON-SUSCEPTIBLE PEOPLE
[I’d skip this one unless you’re interested in knowing how we initially realized that Covid isn’t a threat to healthy young people.]
I mentioned earlier that even without prior exposure to common cold coronaviruses, some people still don’t get Covid-19 after exposure. In other words, some individuals may simply not be susceptible to Covid-19 infection.
Why do some people not get Covid-19 after exposure? To start exploring this, let’s review the attack rate. The attack rate is the number of new cases in the population divided by the number of people at risk.
But what does “at risk” mean? It might seem correct to say that everyone is at risk of Covid-19 infection since no human has interacted with this virus before. However, not everyone is necessarily at risk. In this context, risk does not refer to the likelihood of illness or death after having Covid-19. Instead, it is the likelihood of becoming infected by Covid-19 in the first place.
The percentage of the population at risk definitely isn’t 100%! We understand this because not everyone in a household tests positive after close family exposure. For example, in a close-knit family, sometimes only half of the members test positive after an index case appears. Additionally, you can have Covid-19 on a cruise ship, yet not everyone tests positive. We know how contagious this virus is; it spreads very efficiently from person to person. So, why don’t all exposed individuals end up testing positive for Covid-19? Some people look at the 60–80% attack rate in enclosed settings (like a ship or a prison) and interpret that as indicating herd immunity at 60–80%. But most people don’t live in those crowded environments, so using data this way is incorrect and doesn’t tell us the herd protection level outside of ships and prisons. The key question is: Why don’t 100% of people get Covid-19 after significant exposure? Is it because some people are resistant to getting Covid-19?
First, to an infectious disease physician, that is the wrong use of “resistant.” We use the word resistant when talking about an organism. For example, HIV and bacteria develop drug resistance and become resistant. However, being non-susceptible to an infection is different from being resistant. An organism can be or become resistant to treatment. A human, on the other hand, can be not susceptible to an infection. Specifically, that means, for whatever reason, you don’t get infected after exposure. Next, being non-susceptible isn’t necessarily linked to immunity. There are rare people who lack the cellular receptors that HIV uses to enter cells and who do not get HIV. This is how bone marrow transplants have “cured” HIV. You can transfer these non-susceptible cells through bone marrow transplantation and make HIV go away. Of course, bone marrow transplants are complex and risky, which is why they are not a practical way to cure HIV.
What about for Covid-19? Why do some people get exposed to SARS-CoV-2 and not get Covid-19? This is another way of asking the question of who is at risk for Covid-19. It represents the denominator in the attack rate ratio. Not everyone is at risk. In fact, depending on your age, you may be non-susceptible to Covid-19.
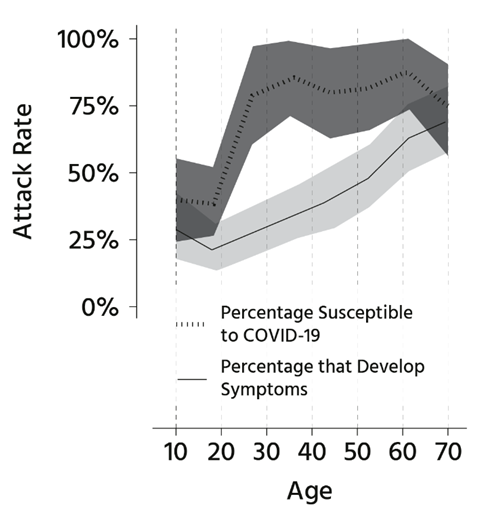
Above, you can see a figure from a paper in Nature Medicine that demonstrates the concept of non-susceptibility. This graph spans the ages of 10 to 70. Unfortunately, data wasn’t collected for people younger or older.
The dotted line separates susceptible individuals from those who are not susceptible to contracting Covid-19. In other words, after exposure to someone with active Covid-19, individuals above the dotted line are resistant, while those below are vulnerable. Note that most young people are initially resistant, but this resistance quickly changes between the ages of 20 and 30. As people get older, approximately 75% of the population remains vulnerable to Covid-19, and this percentage stays consistent.
Next, the solid line indicates those who go on to develop symptoms. The population above the solid line but below the dotted line represents people who are asymptomatically infected after exposure. Those below the solid line are individuals who are symptomatic from Covid-19. Note the slow, steady rise in this solid line. The proportion of people who develop symptoms after exposure increases steadily with age. However, at ages older than 70, about 25% of the population is non-susceptible, with a small proportion being asymptomatic, while roughly 75% develop symptoms.
This is an important concept that involves many details. I want to simplify it and go over it again.
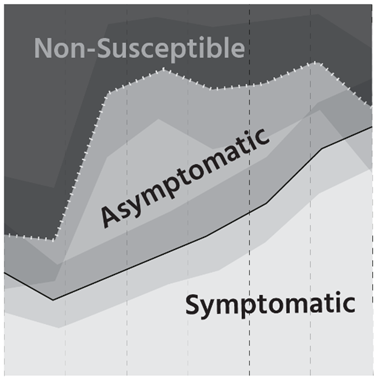
In the figure above, individuals above the dotted line are not susceptible to COVID-19 infection after exposure. This proportion of people changes rapidly around the ages of 20-30. Before that, most are not susceptible. After that, most are asymptomatic. However, as people age, the likelihood of being symptomatic instead of asymptomatic increases linearly.
These figures are approximate and may change over time, but they are significant when considering age and attack rate. For individuals under 20 years old, the attack rate is roughly 20% after exposure. For those over 70 years old, the attack rate is about 70% after exposure.
I would love to learn more about children under 10, since they are a vulnerable group. Newborns have a very different immune system from even six-month-olds, and it continues to develop as they grow. Although there have been outbreaks in daycares, many daycares worldwide have never closed. I suspect that a large percentage of children under 10 are not susceptible. Regarding those over 70, it probably remains around 25% who are not susceptible, but time will tell.
So, we understand that Covid-19 is very effectively transmitted to people. If you have an infected person in a closed room, everyone there should become infected unless they are immune or not susceptible. However, who chooses (or is forced) to be in that room also influences transmission and the attack rate and illustrates the concept of heterogeneous mixing.
I’m Non-Susceptible
What does it mean to be non-susceptible? Why does this change with age? Is it purely an immunological phenomenon, meaning the immune system prevents infection after exposure—either from past infections with coronaviruses or other antigens—or is it a non-immunological process that depends on genetic expression? We know that certain individuals, based on their genetics and how those genes are expressed in their environment, are more or less vulnerable to diseases. Even identical twins with the same genes can respond differently to illnesses depending on their environment. Some people have small variations in their genetic makeup or gene expression that make them less susceptible to Covid-19 infection.
What is clear: Novel infections will exhibit greater variation in susceptibility than non-novel infections. That is, after an infection has been present in a population for a while, it has already had time to cause adverse effects on those who are susceptible. The most susceptible tend to contract the disease and may die from it. Those less susceptible are less likely to get the disease and may constitute a larger portion of the population. With a new virus, the range of susceptibility should be quite broad before the population has been exposed to that infection. Over time, as selective pressure acts and some individuals leave the gene pool, susceptibility probably becomes more uniform across the population.
Will we see Covid-19 alter gene distributions in humans? Unlikely, because advances in modern medicine reduce selective pressures. Additionally, most people who die from Covid-19 are past reproductive age and will not pass on genes that are more or less protective.
Why are some people not susceptible to catching Covid-19 after heavy exposure? I look forward to science providing an answer.
[I asked AI: here are the results from Perplexity]
Several fascinating mechanisms explain why certain individuals appear resistant to SARS-CoV-2 infection despite significant exposure. Research has identified genetic, immunological, and molecular factors that contribute to this phenomenon, revealing a complex interplay of human biology that affects viral susceptibility.
What is clear: Novel infections will have more variation in susceptibility than non-novel infections. That is, after an infection has been present in a population for a while, it has already had time to cause adverse effects on the population susceptible to it. Those most susceptible tend to get the disease and may die from it. Those less susceptible are less apt to get the disease and may become a greater share of the population. With a novel virus, the range of possibilities for susceptibility should be quite large before the population has been challenged with that infection. Later, as selective pressure is applied and some people depart the gene pool, susceptibility likely becomes more consistent across the population.